Hepatopulmonary Syndrome (HPS) is a rare abnormality of the lung which is caused by liver disease. Although not all patients with liver disease get this lung abnormality, patients who do have it can become short of breath and have low oxygen levels.
The problem is that when the liver is not working properly, the blood vessels in the lungs, called capillaries, become enlarged, or “dilated.” Normally, these capillaries carry red blood cells into the lungs, so that oxygen can flow from the lung’s air sacs (“alveoli”) into these red blood cells, which then carry the oxygen to the rest of the body. However, if the capillaries in the lungs become severely dilated, red blood cells are unable to properly absorb oxygen. This is why patients have low oxygen levels and can become very short of breath.
Why do I feel short of breath?
Video Transcript: In a healthy person, red blood cells pass through the small blood vessels in the lungs, picking up oxygen from the air inside the lungs. This oxygen is then able to travel to supply the rest of the body. In hepatopulmonary syndrome the small blood vessels in the lungs become dilated or wider and the oxygen is no longer able to reach all the red blood cells within the vessel. This means that less oxygen is absorbed from the lungs.
Hepatopulmonary Syndrome versus “Pre” – Hepatopulmonary Syndrome
There are 3 basic features that are required to make a diagnosis of hepatopulmonary syndrome:
- Liver disease (diagnosed on ultrasound, cat scan, and/or bloodwork)
- Dilated blood vessels in the lungs (diagnosed with an ultrasound of the heart called an “echocardiogram” with an injection of bubbles called saline contrast at the same time)
- Reduced oxygen levels (diagnosed by taking a sample of blood from an artery, called an “arterial blood gas”)
What if you have only liver disease and dilated blood vessels, but your oxygen levels are normal? In this case, you don’t have hepatopulmonary syndrome, but if your oxygen levels ever did drop, you could develop hepatopulmonary syndrome. We call this “pre-hepatopulmonary syndrome” or “subclinical hepatopulmonary syndrome.” Although this might sound scary, the majority of patients who have this remain stable and do not progress to actually develop hepatopulmonary syndrome. Although not a lot is known and more research has to be done in these patients, for now we simply monitor these patients over time and make sure that they remain stable.
Who Gets Hepatopulmonary Syndrome?
We do know that HPS occurs in about 15% of patients with liver disease of various sorts, but we do not yet clearly understand why some people with liver disease end up with HPS and others do not. HPS is not necessarily seen in patients with more severe liver disease – it can be seen even in patients with mild liver disease. Also, there is no particular cause of liver disease that is associated with HPS. It can be seen in any type of liver disease.
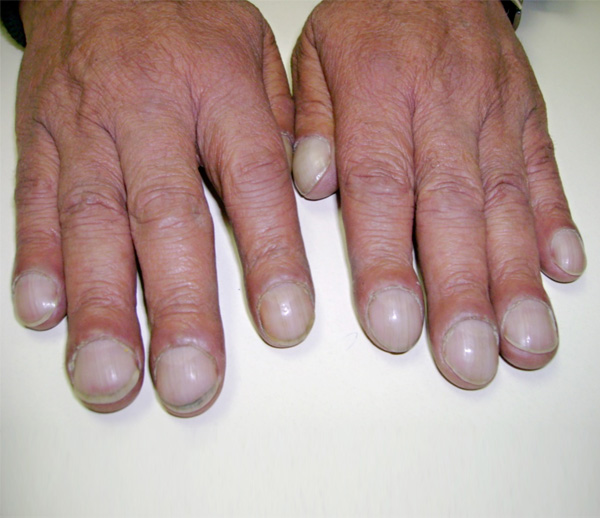
What are the Signs and Symptoms of Hepatopulonary Syndrome?
Hepatopulmonary Syndrome can cause low oxygen levels in your blood. Having low oxygen levels in your blood means people with HPS experience shortness of breath, which can become more and more severe over time. When oxygen is not travelling through your body properly, you may notice that your fingertips turn blue or that your fingernails change shape over time (called clubbing). You may also experience more breathlessness in the sitting or standing position, and feel better when lying flat (this is called “platypnea”). Click and drag the image handles to see the sign of fingernail clubbing.
What is the Prognosis in Hepatopulmonary Syndrome?
The prognosis in hepatopulmonary syndrome is mainly determined by whether or not a liver transplant can be performed. The majority of patients with hepatopulmonary syndrome have gradually worsening shortness of breath and oxygen levels over time, until they get a liver transplant. As time progresses, many patients may require oxygen therapy. When compared to patients who have a similar extent of liver disease but do not have hepatopulmonary syndrome, patients with hepatopulmonary syndrome also tend to have more complications of their liver disease and have a higher chance of dying from these complications. This is why liver transplant is so important. However, there are also some patients who stabilize and can survive for many years with chronically low oxygen levels due to hepatopulmonary syndrome. So far, there is not much research in this population of patients, and more information is required.
What is the Treatment of Hepatopulmonary Syndrome?
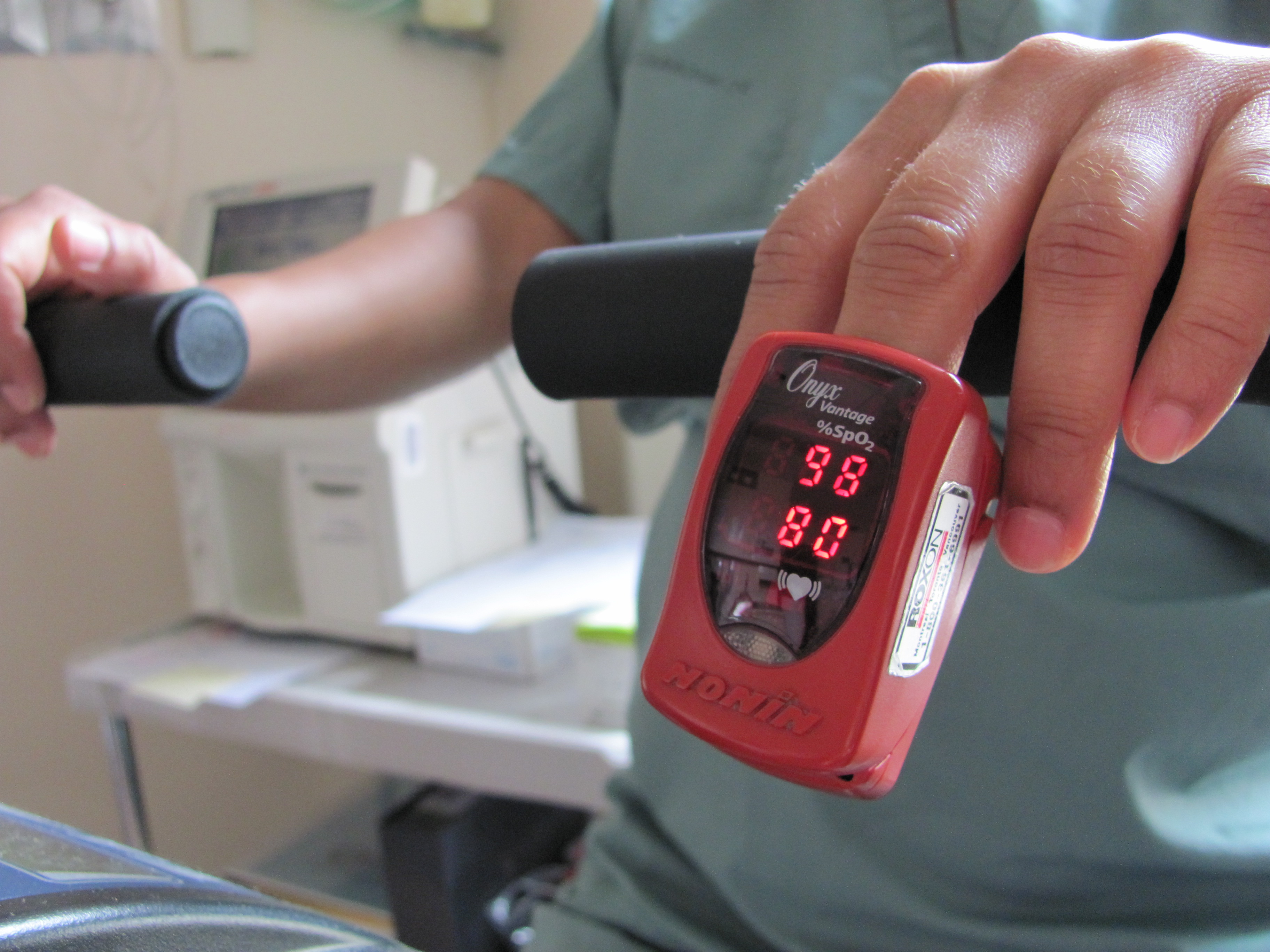
In patients that need it, oxygen treatment is used to increase oxygen levels to make sure that the body’s organs are receiving enough oxygen. Some oxygen may be required even when a patient is at rest, and often more oxygen is required when a patient is moving around. Often, less oxygen is required when a patient is lying down, and more oxygen when he/she is sitting or standing (called “orthodeoxia”). We can test for oxygen levels in the blood stream by placing a device on your finger tip called a pulse oximeter and by taking a blood sample from an artery in your wrist to measure your oxygen levels directly. However, the only cure for HPS is a liver transplant. The new liver begins to repair the damaged lungs, and over a period of weeks to months, most patients’ blood vessels shrink back to the normal size, oxygen levels come back to normal, and shortness of breath disappears. Current research is addressing the following areas of uncertainty: which patients are more likely to have complications after a liver transplant, and why some patients improve faster than others.
Hepatopulmonary Syndrome & Liver Transplants
Currently, the only known effective therapy for HPS is a liver transplant. When the damaged liver is replaced, the majority of HPS patients will gradually experience either significant improvement or complete resolution of blood oxygen levels – and no longer feel short of breath. Although there are no other proven treatment options, there is currently lots of ongoing research to try to find a medicine that can cure hepatopulmonary syndrome, without requiring a liver transplant. This is especially important for patients who do not qualify for a liver transplant. Patients from our Toronto clinic are referred to the Toronto General Hospital (part of the University Health Network) and patients from our Montréal clinic are referred to Hôpital St-Luc (part of the Centre hospitalier de l’universite de Montréal) for liver transplant consultation and procedures. However, our team works closely with patients, their families, and the transplant team to monitor patients before, during, and after the transplant process. If you are already listed for a liver transplant, being diagnosed with HPS may or may not have an impact on your transplant status.
- More information about liver transplants is available on the Canadian Liver Foundation’s website
- More information about liver transplants in Toronto is available on the Toronto General Hospital Liver Transplant website (part of the University Health Network)
- More information about liver transplants in Montréal is available on the CHUM website
The information on this page is based on the latest scientific studies of hepatopulmonary syndrome. You can click on the following references to read the original article.
- Rodriguez-Roisin R, Krowka MJ: Hepatopulmonary syndrome–a liver-induced lung vascular disorder. New England Journal of Medicine 2008;358(22):2378-2387.
- Fallon MB, Abrams GA: Pulmonary dysfunction in chronic liver disease. Hepatology 2000;32(4 Pt 1):859-865.
- Iyer VN, Swanson KL, Cartin-Ceba R, Dierkhising RA, Rosen CB, Heimbach JK, et al. Hepatopulmonary syndrome: favorable outcomes in the MELD exception era. Hepatology 2013;57(6):2427-35.
- Rodriguez-Roisin R, Krowka MJ, Herve P, Fallon MB, ERS Task Force Pulmonary-Hepatic Vascular Disorders (PHD) Scientific Committee. Pulmonary-Hepatic vascular Disorders (PHD). [Review] [281 refs]. European Respiratory Journal 2004;24(5):861-880.
- Krowka MJ, Dickson ER, Cortese DA: Hepatopulmonary syndrome. Clinical observations and lack of therapeutic response to somatostatin analogue. Chest 1993;104(2):515-521.
- Abrams GA, Sanders MK, Fallon MB: Utility of pulse oximetry in the detection of arterial hypoxemia in liver transplant candidates. Liver Transplantation 2002;8(4):391-396.
- Krowka, M. J., Fallon, M. B., Kawut, S. M., Fuhrmann, V., Heimbach, J. K., Ramsay, M. A., … & Sokol, R. J. (2016). International Liver Transplant Society practice guidelines: diagnosis and management of hepatopulmonary syndrome and portopulmonary hypertension. Transplantation, 100(7), 1440-1452.